Comprehensive Insights into the Role of Nurses in Patient Care (Part 2)
Introduction: Nurses play a vital role in patient care, serving as the backbone of healthcare teams. Their collaboration with other healthcare professionals, ethical and legal responsibilities in medication administration, pain assessment and management, infection prevention and control, organization of patient care, stress management, emotional support provision, end-of-life care, advocacy for patient rights, and comprehensive nursing assessments are all critical aspects of their multifaceted role.
In this article, we will explore each of these topics to provide a comprehensive understanding of the invaluable contributions nurses make to the healthcare system. Join us as we delve into the expertise, compassion, and dedication exhibited by nurses in delivering holistic and patient-centered care.

11. How does a nurse collaborate with other healthcare professionals in patient care?
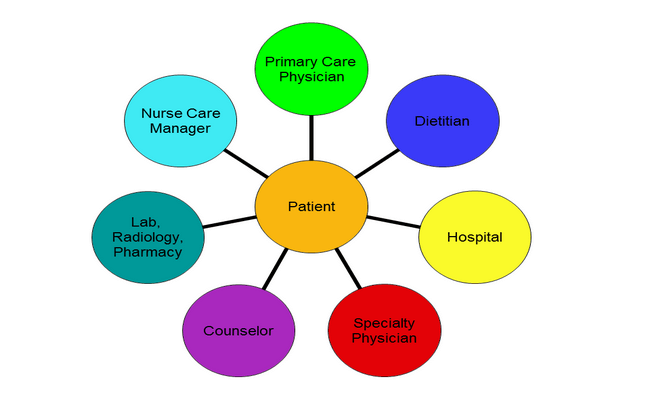
Collaboration is the cornerstone of effective healthcare delivery, and nurses actively engage in interdisciplinary teamwork. Nurses collaborate with physicians, pharmacists, therapists, and other healthcare professionals to ensure seamless patient care. They contribute their expertise, provide crucial insights on patient conditions, participate in care planning, and communicate patient progress.
Nurses coordinate with the healthcare team to implement treatment plans, monitor patient responses, and address any concerns or changes in patient status. Through open communication, mutual respect, and shared decision-making, nurses enhance patient outcomes and promote a holistic approach to care.
12. What are the legal and ethical implications of medication administration by nurses?
Medication administration by nurses carries significant legal and ethical implications. Nurses are responsible for verifying medication orders, ensuring accurate dosages, and administering medications safely. They must have a thorough understanding of medication indications, contraindications, side effects, and potential interactions. Nurses must adhere to legal regulations, organizational policies, and professional standards in medication administration.
They must maintain patient confidentiality, document medication administration accurately, and promptly report any medication errors. Ethically, nurses advocate for patient autonomy, obtain informed consent for medication administration, and prioritize patient safety in all medication-related activities.

13. How does a nurse assess and manage pain in patients?
Assessing and managing pain is a critical aspect of nursing care. Nurses use a comprehensive approach to assess pain, considering the patient’s self-report, physiological indicators, and behavioral cues. They utilize pain assessment tools to quantify pain intensity and monitor its changes over time. Based on the assessment, nurses collaborate with patients to develop individualized pain management plans. This may involve administering appropriate analgesics, implementing non-pharmacological pain management techniques, and providing comfort measures.
Nurses regularly reassess and evaluate the effectiveness of pain management interventions, ensuring patients achieve optimal pain relief and improved quality of life.
14. What is the role of a nurse in infection prevention and control?
Nurses play a crucial role in infection prevention and control, safeguarding patients, healthcare providers, and the community. They adhere to strict infection control protocols, including hand hygiene, proper use of personal protective equipment (PPE), and maintaining a clean and sterile environment.
Nurses educate patients and their families about infection prevention measures, such as proper handwashing and respiratory hygiene. They monitor for signs of infection, implement isolation precautions when necessary, and collaborate with infection control teams to identify and manage outbreaks. By following evidence-based practices, nurses contribute to reducing healthcare-associated infections and promoting patient safety.

15. How does a nurse prioritize and organize patient care?
Effective prioritization and organization are vital skills for nurses to provide efficient and timely care. Nurses prioritize patient needs based on the acuity of their conditions, the urgency of interventions, and the resources available. They assess and triage patients, identifying those requiring immediate attention. Nurses utilize critical thinking to make sound judgments about patient care, ensuring that interventions are appropriately sequenced and delegated.
Organization skills help nurses manage multiple tasks, maintain accurate documentation, and collaborate effectively with the healthcare team. By prioritizing and organizing patient care, nurses optimize patient outcomes and ensure the efficient delivery of healthcare services.
16. What strategies can a nurse use to effectively manage stress in a healthcare setting?
Working in a healthcare setting can be demanding, and nurses face high levels of stress. To effectively manage stress, nurses can employ several strategies. They can practice self-care by prioritizing their physical and mental well-being through regular exercise, healthy eating, and sufficient rest.
Nurses can engage in stress-reducing activities such as mindfulness, meditation, or hobbies that bring them joy. Supportive relationships with colleagues and seeking assistance when needed are crucial. Time management skills, setting realistic expectations, and maintaining a positive mindset can also help nurses cope with stress and maintain their overall well-being.
17. How does a nurse provide emotional support to patients and their families?
Nurses play a pivotal role in providing emotional support to patients and their families during challenging times. They establish therapeutic relationships built on trust, empathy, and active listening. Nurses offer a compassionate presence, providing a safe space for patients and families to express their fears, concerns, and emotions. They provide education and guidance, helping patients and families understand their health conditions, treatment options, and coping strategies.
Nurses also collaborate with social workers, counselors, and support groups to ensure comprehensive emotional support. By addressing the emotional needs of patients and families, nurses contribute to their overall well-being and enhance the healing process.
18. What is the role of a nurse in end-of-life care?
In end-of-life care, nurses play a vital role in providing compassionate and dignified support to patients and their families. They collaborate with the healthcare team and palliative care specialists to manage symptoms, control pain, and maximize comfort. Nurses facilitate effective communication, ensuring patients and families are well-informed and involved in decision-making. They provide emotional support, offer guidance on end-of-life planning, and create a peaceful and supportive environment.
Nurses also assist with spiritual and cultural needs, respecting individual beliefs and practices. By advocating for patient autonomy, ensuring compassionate care, and promoting a peaceful transition, nurses help patients and families navigate the end-of-life journey.
19. How does a nurse advocate for patient rights and autonomy?
Nurses serve as advocates for patient rights and autonomy, ensuring that patients’ voices are heard and respected. They promote informed consent, ensuring that patients understand their treatment options, risks, and benefits. Nurses facilitate communication between patients, families, and the healthcare team, ensuring that patient preferences and values guide care decisions.
They address patient concerns, protect patient confidentiality, and ensure equal access to healthcare services. Nurses act as a liaison between patients and the healthcare system, advocating for fair and equitable treatment. By upholding patient rights and autonomy, nurses empower patients to actively participate in their care and make informed decisions.
20. What are the key components of a comprehensive nursing assessment?
A comprehensive nursing assessment involves gathering holistic information about the patient’s physical, psychological, social, and spiritual aspects. Key components of a comprehensive nursing assessment include:
- – Health history: Collecting information about the patient’s past and current health conditions, medical treatments, allergies, and medications.
- – Physical examination: Assessing the patient’s vital signs, body systems, general appearance, and physical functioning.
- – Psychosocial assessment: Evaluating the patient’s emotional well-being, coping mechanisms, support systems, and cultural considerations.
- – Cognitive assessment: Assessing the patient’s cognitive functioning, memory, orientation, and decision-making capacity.
- – Nutritional assessment: Evaluating the patient’s nutritional status, dietary habits, and hydration levels.
- – Pain assessment: Assessing the presence, intensity, location, and characteristics of pain, as well as its impact on the patient’s well-being.
- – Functional assessment: Evaluating the patient’s ability to perform activities of daily living, mobility, and independence.
- – Risk assessment: Identifying potential risks and vulnerabilities, such as falls, pressure ulcers, or infection.
By conducting a comprehensive nursing assessment, nurses gain a holistic understanding of the patient’s needs, enabling them to develop individualized care plans and promote optimal health outcomes.
Conclusion:
Nurses are indispensable members of the healthcare team, embodying compassion, expertise, and dedication in providing patient-centered care. From collaborating with other healthcare professionals to advocating for patient rights and delivering comprehensive assessments, nurses ensure the well-being and safety of patients.
Their role extends beyond physical care, encompassing emotional support, infection control, pain management, and end-of-life care. By recognizing the diverse skills and responsibilities of nurses, we can appreciate their invaluable contributions to the healthcare system and the lives of those they serve.
IMP LINKS
You can easily find relevant resources and articles on each of the topics mentioned by conducting a search on reputable websites, nursing journals, and databases. Some reliable sources to explore include:
1. PubMed (https://pubmed.ncbi.nlm.nih.gov/):
A widely-used database for biomedical literature, including nursing research and articles.
2. The American Nurses Association (ANA) website (https://www.nursingworld.org/):
The official website of the ANA, which provides resources, publications, and position statements on various nursing topics.
3. Nursing journals such as the Journal of Nursing Scholarship:
(https://journals.lww.com/jns/Pages/default.aspx), Journal of Advanced Nursing (https://onlinelibrary.wiley.com/journal/13652648), and the American Journal of Nursing (https://journals.lww.com/ajnonline/pages/default.aspx), among others. These journals often publish articles related to the different aspects of nursing care.
4. Indian Nursing Council:
Websites of nursing organizations and regulatory bodies, such as the Indian Nursing Council (http://www.indiannursingcouncil.org/) and the Delhi Nursing Council (You can search for their official website using an internet search engine).
Remember to critically evaluate the sources you find and ensure they are reliable, current, and align with evidence-based practice in nursing.
Read More:
- The Role of a Nurse in Healthcare: Providing Compassionate and Essential Care
- A Linguistic Journey: Exploring Abbreviations and Acronyms in the Medical Terminology of Nursing Students | Full forms for the letter ‘A TO Z’
- Decoding the Lexicon: Abbreviations and Acronyms in the Vocabulary of Nursing Students
- Abbreviations and Acronyms: The Language of Nursing Students in Medical Terminology
- From A to Z: The Essential Short Forms Every Medical Student Should Know